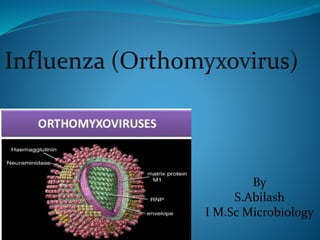
Orthomyxovirus
- 2. Introduction Orthomyxoviridae is a family of RNA viruses. It includes seven genera: Influenzavirus A, Influenzavirus B, Influenzavirus C, Influenzavirus D, Isavirus, Thogotovirus, and Quaranjavirus. The first four genera contain viruses that cause influenza in vertebrates, including birds, humans, and other mammals.
- 3. Scientific name: Orthomyxoviridae Higher classification: Negative-sense single- stranded RNA virus Rank: Family Class: Insthoviricetes Order: Articulavirales Phylum: Negarnaviricota Lower classifications: Influenza A virus, Influenza B virus, Influenzavirus C, Bourbon virus, Isavirus
- 4. General classification Orthomyxoviruses are large, enveloped virions with helical nucleocapsids. Negative sense, segmented RNA genomes. Pleomorphic: laboratory strains are often spherical, whereas clinical strains are often filamentous. Replicate in the nucleus. Upon budding, the host cell is killed.
- 5. Conti.... Influenza viruses A, B, and C are pathogenic in humans Influenza A and B are responsible for most illnesses and epidemics. Influenza A also infects non-human mammals and birds, which facilitates zoonotic infections.
- 7. Antigenic changes: – Minor changes include mutations, which can lead to genetic drift and epidemics; both influenza A and B undergo these kinds of changes. – Major changes include re-assortment, which can lead to genetic shift and pandemics; influenza A virus is associated with pandemics. – Reassortment occurs when viruses with segmented genomes create a hybrid strain. – An example of this is the H1N1 pandemic strain that arose in 2009; this strain contained genetic information from avian, human, and swine influenza viruses. Host immune response involves cytokine storms and interferons that are largely responsible for the symptoms of the flu.
- 8. Virion Components & Their Functions: Nucleocapsid Lining – Matrix protein (M1) promotes virion assembly. Envelope – Membrane protein (M2) facilitates viral uncoating and release from the host cell; it does so via formation of proton channels that allow for acidification, which is necessary for membrane fusion. – Amantadine and rimantadine target M2 of Influenza A, thus blocking viral uncoating.
- 10. Virion Components & Their Functions: Envelope glycoproteins – Hemagglutinin acts as a viral attachment protein; it binds sialic acid on epithelial cells (there are a couple of exceptions). Also acts as a fusion protein, attaching the viral envelope to the host cell membrane. Elicits a neutralizing antibody response. Subtypes determine the species and tissue type that the virion can infect. – Neuraminidase Facilitates virion release from the host cell by cleaving sialic acid. Anti-viral drugs zanamivir and oseltamivir act on neuraminidase to block virion release. Neuraminidase has other functions, which may include liquefaction of the mucous covering of the respiratory tract.
- 12. Key steps of influenza pathogenesis: The virus reaches the mucosal epithelia via respiratory droplets. – The virus can also be transferred to mucosal surfaces via other mechanisms; for example, the virus can be picked up from counters, keyboards, and other hard surfaces, then transferred to the nasal mucosa from the hands. As showed earlier, the virus uses sialic acid receptors on host epithelial cells to gain access to host cells for replication.
- 13. Replication primarily occurs in the tracheobronchial tree. Infection triggers release and recruitment of inflammatory cytokines, type 1 interferons, and pro- inflammatory cells. In turn, the adaptive immune system is triggered, and T-cells are activated and antibodies are produced. – These agents provide future protection against re- infection by the same influenza strain.
- 14. Infected epithelial cells are destroyed by budding virions, cytokines, interferons, and other anti-viral agents. – Destruction of epithelial cells also removes the mucosa and cilia that would otherwise provide a physical barrier against pathogens. Symptoms of influenza include fever, headache, cough, chills, muscle pain, sore throat, sinus congestion, and others; again, indicate that these symptoms are primarily caused by the host immune response.
- 16. Complications: In some individuals, complications from the flu can be life- threatening. Pneumonia can result from viral infection or from secondary bacterial infections. Organ inflammation or failure can occur. Sepsis. Indicate that individuals at higher-risk for these complications include those with compromised immune systems, particularly: Very young children (under the age of 5) Pregnant women and women less than two weeks' post-partum Adults over the age of 65
- 18. Diagnosis Based on the symptoms ElISA Cell line culture Immunodiffision Heamagglutination
- 19. Host defense Interferon appears in respiratory secretions shortly after viral titers reach their peak level, and may play a role in the subsequent reduction in viral shedding T cells and antibody-dependent cell-mediated cytotoxicity also participate in clearing the infection.
- 20. IgG antibody, which predominates in lower respiratory secretions, appears to be the most important. The IgG in these secretions is derived from the serum, which accounts for the close correlation between serum antibody titer and resistance to influenza. IgA antibody, which predominates in upper respiratory secretions, is less persistent than IgG but also contributes to immunity.
- 21. Prevention & Treatment: It is difficult to avoid the flu in part because individuals begin shedding the virus before symptoms appear. Flu vaccine is the best way to prevent the flu. – Seasonal vaccines are tailored to protect against strains that are predicted to be most common in a given season. – Most are three component vaccines (aka, trivalent), which means they protect against two strains of Influenza A and one strain of Influenza B. – Four component (aka, quadrivalent) vaccines are also available; they protect against the same strains as the trivalent vaccine and an additional strain of Influenza B. – The vaccines can prevent the flu or, if unable to provide complete protection, they can reduce the severity of symptoms and the likelihood of developing complications. Patients with influenza may be given antivirals to reduce symptom severity and the likelihood of complications